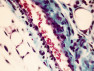
Looking closely at lungs
When you get a cut on your finger, the skin will heal on its own. Why wouldn’t the same thing be possible for lungs? That is what lung researcher Reinoud Gosens wants to find out.
Last week, the Lung Fund started raising money for his research into lungs’ ability to heal themselves.
Tissue regeneration is dependent on wnt growth factors, a protein secreted by the so-called progenitor cell, which prompts the division of nuclei.
A patient suffering from COPD has two problems: they have very few progenitor cells and the growth factor’s signal is distorted.
By subduing the enzyme GSK3 – which slows down cell growth – Gosens was able to activate the nuclei in lung cells anyway.
The next step is to see if these are the correct nuclei and whether the lung tissue actually regenerates. He also has to research whether or not that cell division could get out of hand and become cancer.
But Gosens is convinced he is on the right track when it comes to finding a treatment for COPD: ‘I can see the pieces of the puzzles fitting together.’
Reading time: 8 minutes (1,554 words)
Lungs are wondrous organs. On the one hand, they are amazingly efficient: even when a serious case of COPD has turned them into a spider web of destroyed tissue that is only hanging together by a thread, they still work to help the patient breathe.
On the other hand, their self-healing abilities are minimal, especially in the case of COPD patients. When you cut your finger, your body immediately gets to work to repair the damage. When you cut off half your liver, it will regrow. But your lung? Once it is destroyed, that’s it.
That is really quite strange, says UMCG lung researcher Reinoud Gosens. Why is it that lungs are unable to heal themselves properly? And, as a follow-up question, is there anything we can change about that?
Puffed-out cheeks
His quest for an answer got support last week from a veritable army of Duch celebrities who are ‘holding their breath’ in the fight against COPD. Giel Beelen, Ronald de Boer, Annette Gerritsen: they are all on YouTube and the Lung Fund’s website with puffed out cheeks. They are trying to show that this is how a COPD patient feels every day, when they are fighting for air. They are asking for a donation to the Lung Fund of ten cents for every second you can hold your breath.
Hopefully, this will provide Gosens with the means to continue on a new and exciting path: getting the body to repair lung damage itself.
‘Normally, the body does that with the help of the so-called wnt growth factors’, Gosens explains. ‘These are proteins produced by progenitor cells – a type of stem cell that is slightly more specialised. They send out a signal that tells the nucleus to start dividing and thereby repair the damage.’
Lung attack
But COPD patients suffer from two problems: the lungs contain very few of those progenitor cells – a lot fewer than, for instance, the intestines. Moreover, the chronic inflammation of the airways ensures that that weak signal to the nuclei is distorted as well. So even the progenitor cells that are present are hardly able to do their job. And that is why 6,000 people die of a ‘lung attack’ annually.
Gosens thought there were two things you could do to solve the problems. You can either try to tackle the amount of progenitor cells, or you figure out how to fix the distorted signal. ‘I believe the pharmaceutical route is the most promising’, says Gosens. ‘The body knows how everything works. It just needs a push in the right direction.’
Number one cause of death
Reinoud Gosens says they are in dire need of extra money for lung research. No less than three lung diseases are in the top ten of global causes of death. Every year, COPD kills 3 million people, but if you add lung cancer and pneumonia, that number comes to 7.7 million. That is more deaths than those caused by cardiovascular diseases.
And yet the lung diseases receive much less funding, says Gosens. ‘That’s probably because COPD is often the result of smoking’, says Gosens. ‘People probably feel that someone who suffers from it only has himself to blame.’
He doesn’t think that is right. Among COPD patients, 20 per cent never smoked. There are also victims in developing countries: people who cook over an open fire indoors. But even more importantly, ‘It’s not just to blame people for their lifestyle. Lifestyle also plays an important part in cardiovascular diseases, and many other afflictions as well. We don’t blame people for that, either.’
He thinks he knows where to look for the answer, but that insight is based on fairly recent studies. For a long time, people thought that lungs were entirely incapable of self-healing. ‘But that’s completely impossible’, Gosens explains. ‘When you’re out and about, when you’re alive, your lungs are continuously being damaged by small inflammations, colds, and air pollution. If that didn’t heal, we wouldn’t be alive.’
The first results
The discovery of progenitor cells and wnt growth factors illuminated how the body repairs damage, but those kinds of studies were mainly focused on the intestines. That is because they are excellent at repair. ‘You completely replace your intestines’ epithelial cells in seven days time. They are the layers of cells on the inside’, says Gosens. This feat requires a lot of progenitor cells and growth factors, and that makes them easy to find. But it was not until five years ago when they were finally discovered in the lungs.
When Gosens heard about this, he wasted no time. He set up a study that focused on tissue regeneration in the lungs – the most logical way to fight COPD, he thinks. Now, a year after he started his research, he has the first results: proof that the so-called GSK3 inhibitors clearly activate the nuclei of lung tissue.
‘We already knew that the enzyme GSK3 played a key role in the signal transfer of growth factors’, says Gosens. ‘To be exact: it blocks that transfer.’ Normally, that block serves a function. After all, you do not want the cells in your body to divide without limit. ‘That would be cancer.’ But in the case of lung damage, a bit more cell division would be nice.
Pioneering research
Gosens did experiments with lung slices, wafer-thin pieces of living lung tissue. Next, he made those slices ‘sick’. He affected the tissue’s elasticity by adding elastase, mimicked the damage done by smoking or inflammations with peroxide and finished the whole thing with cigarette smoke extract. He finally added a GSK3 inhibitor to see what would happen.
The result? His data clearly shows that the genes in the nuclei are activated. This gives hope, and is reason for the Lung Fund to call this research ‘pioneering’. But, Gosens warns, we are not there yet. He is not even sure if the GSK3 inhibitors are even the right solution. ‘One lung slice contains 42 different cells’, he says. ‘We can see that genes are more expressive – more prone to division – but we’re not exactly sure which ones they are and what the result is.’ A gene does not lung tissue make, so to speak.
The next step is to determine exactly which cells become active after the GSK3 inhibitors have been added. This research is fully under way. ‘It is literally happening in a laboratory down the hall.’ Gosens hopes to have the results from this research in approximately two months. ‘If we can prove that the GSK3 inhibitors actually promote cell growth, then we have proof of concept’, he says. That would be a huge step.
Next, he wants to find out what GSK3 inhibitors would do in a living organism. For that, he needs mice who are specifically suffering from lung damage similar to COPD. Next, he will be staining the progenitor cells in those lungs so that he can track exactly how the progenitor cell develops into possible new lung tissue.
Countless obstacles
He admits that his research looks especially promising, but there are still countless obstacles: a lung slice is no lab animal, and what works in a mouse does not necessarily work in a human being. And even if it does work, you still have to see if there are any side effects: you do not want the tissue regeneration to get out of hand, causing cancer while you are trying to cure COPD. ‘That is very complex and costs an enormous amount of money’, says Gosens.
However, one GSK3 inhibitor is very well-known and has been on the market for years: lithium. It is prescribed to people suffering from bipolar disorder. ‘It seems to have very few side effects’, he says. ‘It would be interesting to see what it can do for people suffering from COPD.’
In addition to his research into GSK3, Gosens is going even further. Blocking this enzyme was obvious, but perhaps there are even better ways. ‘I’m not ruling any of that out.’
For now, he knows one thing for sure: he is on the right path. ‘I can see the pieces of the puzzle fitting together’, he says. ‘But I have no idea if the puzzle has a hundred, a thousand, or ten thousand pieces.’
Hold your breath
Last week, the Lung Fund launched the campaign ‘Hold your breath’. Giel Beelen, Ronald de Boer, and other Dutch celebrities challenge people to hold their breath for as long as they can and donate ten cents for every second. The Lung Fund hopes to raise 300,000 euros for Reinoud Gosens’ study.
The campaign went ‘live’ on Thursday ,18 February. So far, houjeademin.nl has a scant 13,000 ‘seconds’, or, in other words, 1,300 euros. Not a bad start, says Lung Fund spokesperson Jelmer Krom. ‘Those are the seconds from the videos that were uploaded to the site’, he explains. ‘And we can see people are starting to challenge and tag each other on social media. You have to give it time to spread.’
The campaign has no end date. ‘We’ll continue until we’ve raised 300,000 euros.’